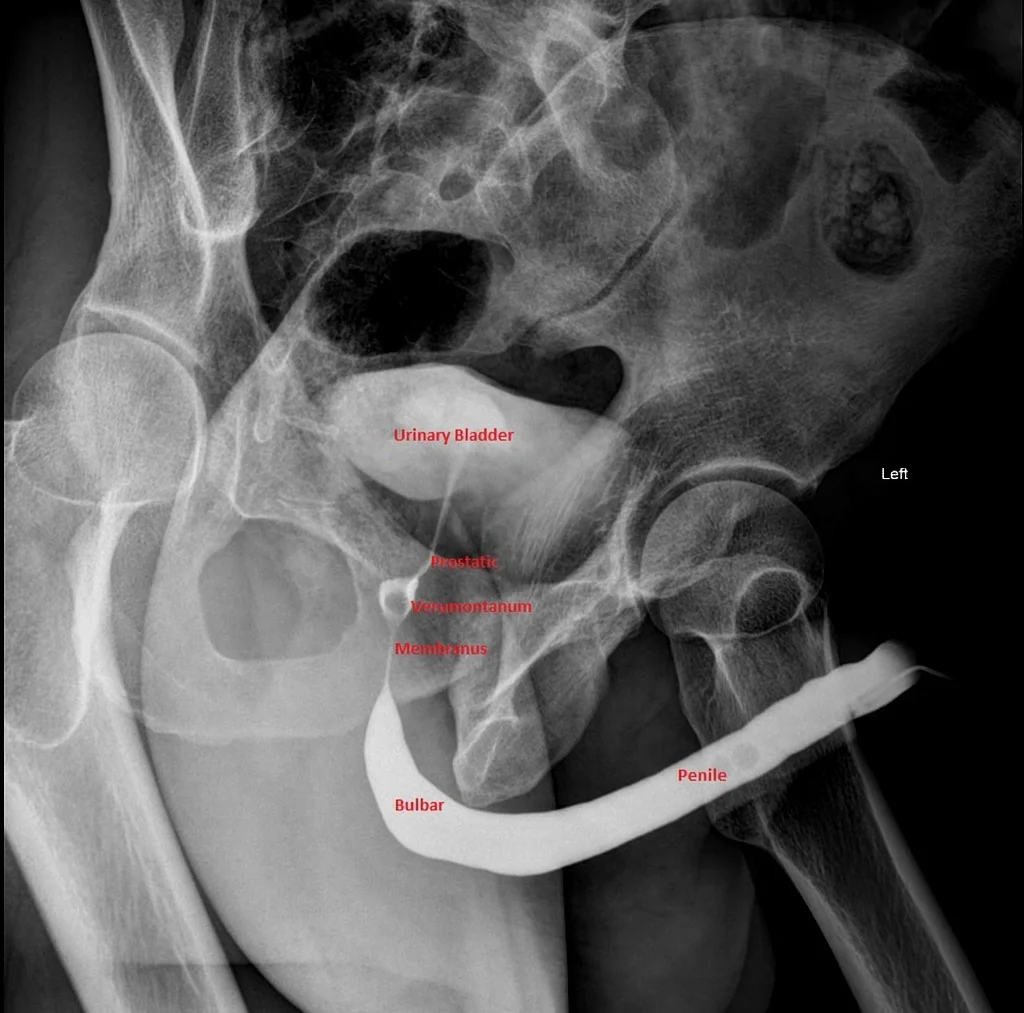
The Importance of the RUG
/It is early on in your residency training, when you receive sign-out of a patient who was involved in an MVC with multiple injuries including a stable pelvic injury. The patient, a middle-aged male, has not voided three hours into his visit and there is no mention of any obvious genital trauma. He has had a negative FAST exam in addition to the rest of your primary and secondary assessment. The patient mentions to the nurse that he is trying to urinate but cannot void and has some discomfort. The bladder scan shows that the patient has about 500cc of urine and when the nurse goes to place a urinary catheter she pauses as she sees what appears to be dried blood at the urethral opening. After reassessing the patient who is still hemodynamically stable with normal mentation, his findings are discussed with Urology who recommend getting a retrograde urethrogram prior to any additional procedures.
Read More