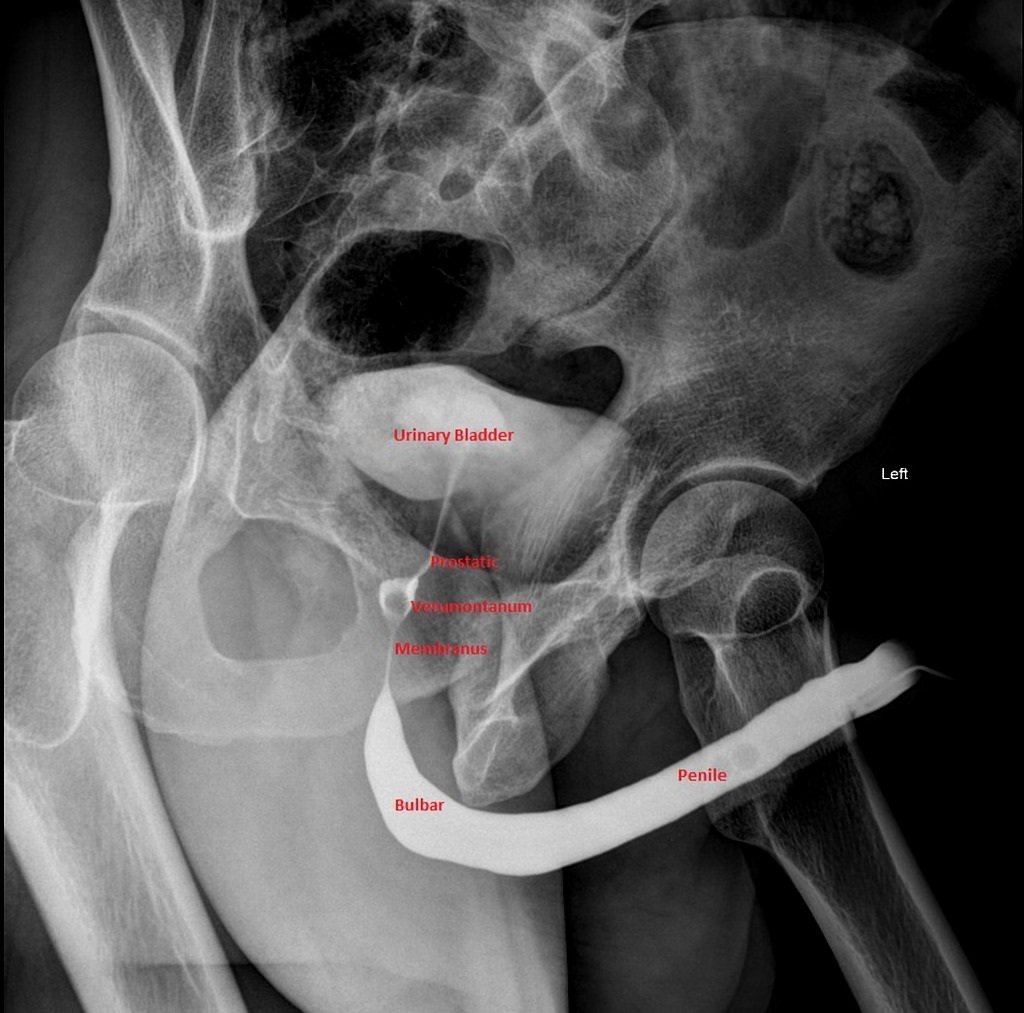
The Importance of the RUG
/Case courtesy of Dr Mohammad Taghi Niknejad, https://radiopaedia.org/cases/61843"
As with any trauma, stabilizing life-threatening injuries takes priority. Following the stabilization of these injuries, attention should turn to the evaluation and management of conditions that have significant morbidity including urethral injury. A retrograde urethrogram (informally known as the “RUG” and also referred to as an ascending urethrogram) is a test ordered for suspected urethral injury and was first described in the literature in the early 1900s. (1, 2)
To understand how to diagnose urethral injuries, a quick review of the anatomy of the urethra is important. The urethra is divided into anterior and posterior portions. The anterior urethral portion is typically five times the length of the posterior urethra. Since the length of the anterior urethral portion is much longer, injuries to this portion of the urethra are more common than the posterior urethra. Isolated blunt injuries to the penis such as a kick to the groin, penile fractures, straddle injuries will likely be the mechanism of injury to the anterior urethra. (3) The posterior urethra rarely has isolated injuries and will typically be injured in cases where there is a pelvic fracture. An expanded list of common mechanisms is listed below in Table 1.
Table 1 - Common Mechanisms of Injury in Urethral Trauma. Chapple C, Barbagli G, Jordan G. Consensus statement on urethral trauma. BJU Int. 2004; 93(9):1195–20
In females, the length of the urethra is much shorter than in males, less externally located and more elastic. As such, it is rare for isolated injuries to the urethra to occur in female patients. To that end, pelvic trauma is the most common mechanism of urethral injury in females and can be associated with bladder rupture, vaginal and rectal trauma. (4,5) The National Data Trauma Bank, over a period of four years, saw that the rates of bladder injury with pelvic traumas in males and females was about the same at 3% but the incidence of urethral involvement in these injuries was tenfold in males at 1.54% vs 0.15% in females. (6)
Indications
The common indications for a retrograde urethrogram are pelvic trauma with suspicion for urethral injury, concern for urethral obstruction, foreign bodies in the urethra, urethral diverticula, or suspected urethral fistula. (1) Though the test can be conducted for multiple urethral pathologies, the cases seen in the emergency department are usually acute and secondary to some form of trauma. The types of trauma seen can range from high velocity accidents (vehicular trauma, falls etc.) penile fracture, and instrumentation of the penis (both iatrogenic and/or self-generated). In trauma (both blunt and penetrating), the presence of blood at the urethral meatus is the most common indication to get the study. In this situation any attempt to place a catheter should be withheld until further testing as to avoid worsening any injury that may be present. It is important to evaluate for any rectal trauma as well and check for a high riding prostate with a rectal exam.
With other traumatic mechanisms such as penile fracture, the patient might present with gross hematuria in addition to ecchymosis, pain and edema of the penis. If there are concerns of abdominopelvic or genitourinary injury, any attempt to place a catheter that is met with resistance should raise the suspicion for urethral injury and a retrograde urethrogram should be considered in addition to involving Urology in the patient’s care.
Diagnosis
In our department, while this procedure can be done at bedside by Urology, it is commonly conducted by radiology technicians. Slight variations exist between different institutions as to how exactly the procedure is performed, but generally speaking contrast media is injected into the urethra in a retrograde manner and a series of radiographs are obtained. In evaluating genitourinary trauma, the two big bodies that provide recommendations/guidelines are the American Urology Association (AUA) and the European Association of Urology (EAU). The radiographic recommendations in trauma that both organizations use are set forth by the American Association for the Surgery of Trauma (AAST) organ injury severity system. Unfortunately Grade A Level of evidence with urethral trauma is rare and most of the recommendations are thus based on Grade B and Grade C. The AUA gave the RUG a Grade C recommendation while the EAU gave it a Grade B rating. (4)
To diagnose an injury to the urethra and give an adequate diagnosis, a voiding cystourethrogram (VCUG) in addition to the RUG will evaluate the vesicourethral junction and determine if there has been any damage to the bladder itself and allow for evaluation of the posterior urethra. Abnormal findings indicative of potential urethral injury includes extravasation of contrast, or an inability for the contrast to enter the bladder secondary to some urethral obstruction. If the RUG shows urethral injury, is equivocal, resistance is met with advancement of the Foley or severe pain is produced, the Foley is NOTadvanced and urologic consultation is obtained.
When interpreting the RUG, there are two grading systems that have been developed. The Goldman classification of urethral injuries is more widely accepted than the AAST grading of urethral injuries. The Goldman classification is based on the anatomical location of urethral injury. The AAST is based on the type of treatment required and degree of disruption in the urethra irrespective of injury location. (5)
Table 2 - Goldman’s Classification of Urethral Injury (1)
Case courtesy of Dr Mohammad Taghi Niknejad. https://radiopaedia.org/cases/61673
The higher grades of injury complete disruptions of the urethra, account for 65% of all urethral injuries while incomplete injuries have been seen in 35% of cases. (8) In the figure below contrast can be seen extravasating from the urethra.
In trauma centers, most trauma patients require some hemodynamic support and frequently with large volume resuscitation. In these cases, a Foley catheter is placed to adequately monitor intake and output. In patients who might have urethral injury this can be missed for some significant amount of time. While the CT is not primarily used to diagnose urethral injury, there are some CT findings that are seen with a higher frequency in patient with urethral injuries than those without. These are summarized in Table 3. (9)
Table 3 - Common CT findings seen with urethral injuries
Urethral ultrasound has been studied for the evaluation of urethral strictures but few studies have evaluated its value in the evaluation of urethral trauma. However, sonographic findings such as bilateral hydronephrosis and blood clots in the bladder should raise suspicion for lower genitourinary injury. The RUG has been shown to be better at evaluating the anterior urethra but very poor at showing the posterior urethra. This is better visualized by the VCUG which is conducted after a normal RUG as the site of injury is in the proximal portion of the urethra. Flexible cystoscopy can be used in instances where the visualization of the bladder and posterior urethra are indeterminate with the RUG and VCUG.
Complications/Limitations
There are no absolute contraindications to performing a RUG. The only relative contraindication is in patients who are allergic to radiopaque contrast. However, the risk of allergic reaction is low as the probability of contrast gel accessing the vascular space is relatively small. Depending on the reaction, one can pre-medicate accordingly following institutional protocols. The most frequent reported complications are reaction to the contrast, development of urinary tract infection and discomfort to the patient. (10) A retrospective study over 10 years found no evidence of increased risk of UTI’s in patients receiving urethrograms. (11) The most common limiting factor of the study is poor technique. Care is taken to avoid spilling contrast which may result in a false positive or equivocal test.
Conclusion
To keep up with the time sensitivity that most trauma patients present with, the RUG has been shown to not only be an efficient test but to be the primary modality and most efficacious test in evaluating patients who have concerning findings of urethral injury. It is a test that is readily available in locations with radiology capabilities and can be quickly done in the department. While it is not considered one of the life-saving imaging studies we do in the department, it’s impact on the morbidity of your patient can be life changing. Its utility in early diagnosis is essential and in collaboration with additional studies can pave the way to early urethral injury management.
References
https://radiopaedia.org/cases/normal-retrograde-urethrogram-rug-and-voiding-cystourethrogram-vcug. Accessed December 9th, 2018
Cunningham JH. The diagnosis of stricture of the urethra by Roentgen rays. Trans Am Assoc Genitourin Surg 5.0 (1910): 369-371.
Chapple C, et al. Consensus statement on urethral trauma. BJU International. 93.9 (2004): 1195–1202. https://www.ncbi.nlm.nih.gov/pubmed/15180604
Bryk DJ, et al. Guideline of guidelines: a review of urological trauma guidelines. BJU International. 117.2 (2016): 226-234. https://www.ncbi.nlm.nih.gov/pubmed/25600513
Ingram M, et al. Urethral Injuries after Pelvic Trauma: Evaluation with Urethrography. RadioGraphics 28.0 (2008): 1631–1643 https://www.ncbi.nlm.nih.gov/pubmed/18936026
Patel DN, et al. Female urethral injuries associated with pelvic fracture: a systematic review of the literature. BJU Int 120.6 (2017): 766-773 https://www.ncbi.nlm.nih.gov/pubmed/28805298
Lynch TH, et al. EAU guidelines on urological trauma. Eur Urol. 47.1 (2005): 1-15. https://www.ncbi.nlm.nih.gov/pubmed/15582243
Zaid UB et al. Penetrating Trauma to the Ureter, Bladder, and Urethra. Curr Trauma Rep 1.2 (2015): 119-124 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4662570/
Ramchandani, P., Buckler PM. Imaging of genitourinary trauma. AJR AM J Roentgenol. 192.6 (2009) 1514-1523 https://www.ncbi.nlm.nih.gov/pubmed/19457813
Maciejewski, C., et al. Imaging of urethral stricture disease. Translational andrology and urology 4.1 (2015): 2-9. https://www.ncbi.nlm.nih.gov/pubmed/26816803
Malhotra NR, et al. Urinary tract infection after retrograde urethrogram in children: A multicenter study. Journal of Pediatric Urology 13.6 (2007):623 https://www.ncbi.nlm.nih.gov/pubmed/28666918
Written by: Edmund Irankunda, PGY-1, University of Cincinnati Department of Emergency Medicine
Peer Review and Editing by: Jeffery Hill, MD MEd