Global Health Case Files #2
/Imagine: you are the single provider manning a rural clinic in Northern Tanzania along the shore of Lake Victoria. You are one of only a handful of physicians in the entire region and you have minimal access to diagnostics or therapeutics. Your clinic does not have any power. Your diagnostics include: urinalysis, urine pregnancy, CBC and rapid tests for HIV, syphilis, and malaria. You have 2 nurses, one of whom acts as a translator (from Swahili to English). You are armed primarily with your intellect, knowledge of local disease processes, and your keen sense of intuition.
Case #5
32 yo M PMH HIV p/w LLE >RLE swelling & pain x 1 year. Recent HIV+ and recently started ARVs. CD4=40. Pt denies trauma. No history of DM or CHF. No fevers, chills, N/V, abd pain, diarrhea.
PE: 37C HR-86 BP-124/82 RR-12
Gen: Grossly abnormal & enlarged LLE. No acute distress.
HEENT: PERRL, EOMI, No conjunctival pallor. Oropharynx clear, no thrush. Significant, diffuse lymphadenopathy. Palpable pre-auricular, submandibular, occipital, anterior cervical, supra/infraclavicular, axillary, and inguinal lymph nodes.
C/V: S1S2 present, RRR, no m/r/g
Resp: CTAB, no crackles/wheezes
Abd: soft, nt/nd, no rebound or guarding
Ext: Grossly enlarged LLE. Diffuse swelling & edema with mild pitting LLE up to thigh. Foot massively enlarged. Mild skin eruption with drainage of serosanguinous fluid. RLE enlarged with mild edema, non-pitting. Pt ambulatory but with some difficulty. The image provided is similar to this patient’s condition.
What is the most likely diagnosis?
Diagnosis = Lymphatic Filariasis
Filariasis is a parasitic disease caused by nematodes (roundworms) transmitted by mosquitoes or black flies. Lymphatic filariasis is caused by the worms Wuchereria bancrofti, Brugia malayi, and Brugia timori. The most striking symptom of lymphatic filariasis is elephantiasis, characterized by thickening of skin and massive edema secondary to lymphatic obstruction by parasites. The other type of filariasis (not our patient), called Subcutaneous filariasis is caused by Loa loa (aka “eye worm”), Mansonella streptocerca, and Onchocerca volvulus. Onchocerciasis is also known as “river blindness” and is second in the world only to trachoma as an infectious cause of blindness.
Filariasis affects 120 million people and is considered endemic in 73 countries, 37 of these in Africa. First line treatment is albendazole + ivermectin in Sub-Saharan Africa while albendazole is used with diethylcarbamazine (DEC) in other countries. We did not have ivermectin or DEC so we used albendazole + doxycycline (for 6 weeks).
Case #6
25 yo M (never immunized) p/w abdominal pain/distension and mucus in stool x 3 weeks. No fevers, chills, nausea, vomiting. +lethargy.
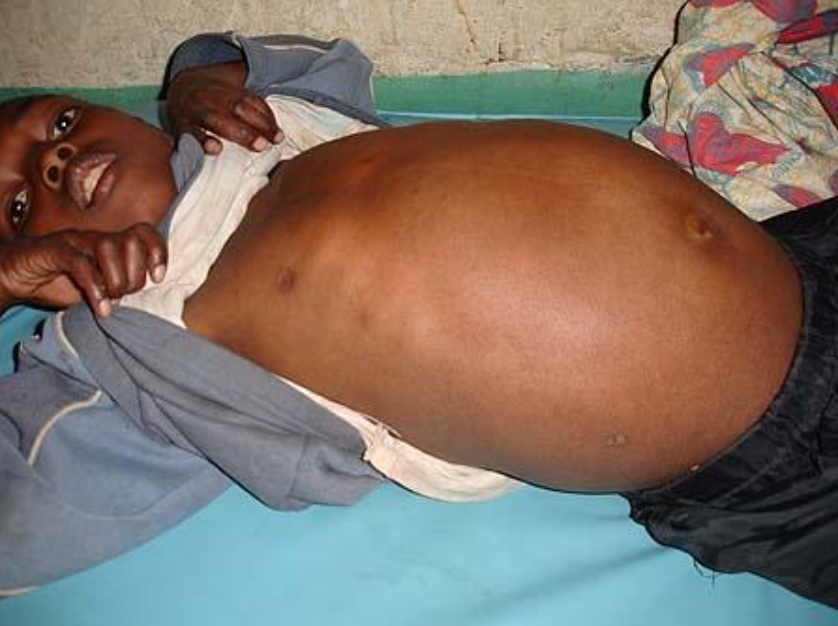
Normal vitals, appears chronically ill. Significantly jaundiced with scleral icterus. Exam notable for massive hepatomegaly, measuring approximately 18x 25cm below the costal margin. Firm, nodular, non-tender to palpation, extends to the RLQ below the umbilicus and also to the LLQ. Images below.
What is the most likely diagnosis and what is the likely etiology?
Diagnosis = Hepatocellular carcinoma (2/2 to Hepatitis B)
In countries where immunization rates are low, endemic hepatitis B is the predominant cause of hepatocellular carcinoma (HCC). In the U.S. where hepatitis B is rare because of high vaccination rates, the major cause of HCC is cirrhosis, usually due to alcohol abuse. Prognosis is poor because only 10-20% of hepatocellular carcinomas can be removed completely with surgery. Also, a majority of cases occur in resource-limited settings. Median time to death is often 3-6 months.
Case #7
18 yo M local fisherman no sig PMH p/w abdominal pain/swelling, epistaxis and pyrexia to T 40C.
Extensive splenomegaly with spleen extending to RLQ. Hb 7.5. Abdominal U/S shows large homogenous spleen without mass or abscess; significant for portal vein dilatation. Pt elopes prior to further labs/testing obtained.
What is the most likely diagnosis?
Diagnosis = Acute Schistosomiasis (aka Katayama Fever)
Schistosomiasis (also known as Bilharzia) is a parasitic disease caused by several species of trematode belonging to the genus Schistosoma. Snails serve as the intermediary agent between mammalian hosts (humans, cattle, sheep, goats, etc). Disease is spread primarily by exposure to water contaminated by infected snails (in this case Lake Victoria) and is very common within developing countries where water sanitation is poor. Schistosomiasis affects approximately 210 million people worldwide, 85% of whom live in Africa. It is the second most socioeconomically devastating parasitic disease after malaria.
Schistosomiasis is a chronic disease, often subclinically symptomatic, with mild anemia and malnutrition. Acute Schistosomiasis (Katayama Fever) may occur several weeks after the initial infection and presents with fever, abdominal pain, hepatosplenomegaly, diarrhea, fatigue, and eosinophilia . It may also present with portal hypertension leading to splenomegaly and hematemesis. The primary treatment is praziquantel. Schistosomiasis is also becoming increasingly prevalent among travelers, so a high level of suspicion must be kept for patients returning (usually 1-8 weeks) after contact with fresh water and developing signs/symptoms such as fever, rash, hepatosplenomegaly, or eosinophilia.
References
- WHO: Regional Office South-East Asia. The Regional Strategic Plan for Elimination of Lymphatic Filariasis, 2010-2015.
- CDC. “Hepatitis B” Prevention Epidemiology and Prevention of Vaccine-Preventable Diseases, 13th edition. 2015.
- Mazigo et al. Epidemiology and control of human schistosomiasis in Tanzania. Parasites & Vectors 2015; 5:274.

![Dr. F. W. O’Connor. CC BY 4.0 (http://creativecommons.org/licenses/by/4.0)], via Wikimedia Commons](https://images.squarespace-cdn.com/content/v1/53c1a2cce4b0e88e61f99b70/1440782855563-VUJHLH69T6AZDNCHP0Q8/image-asset.png)
![Anand Selvam. CC BY 4.0 (http://creativecommons.org/licenses/by/4.0)], via Wikimedia Commons](https://images.squarespace-cdn.com/content/v1/53c1a2cce4b0e88e61f99b70/1440783052180-8YGIM8YW6V270QO7PBSX/image-asset.png)
![Anand Selvam. CC BY 4.0 (http://creativecommons.org/licenses/by/4.0)], via Wikimedia Commons](https://images.squarespace-cdn.com/content/v1/53c1a2cce4b0e88e61f99b70/1440783080885-CDV73BFUYU1DWD2HSYZ2/image-asset.png)