Annals of B-Pod: To Cric or Not to Cric?
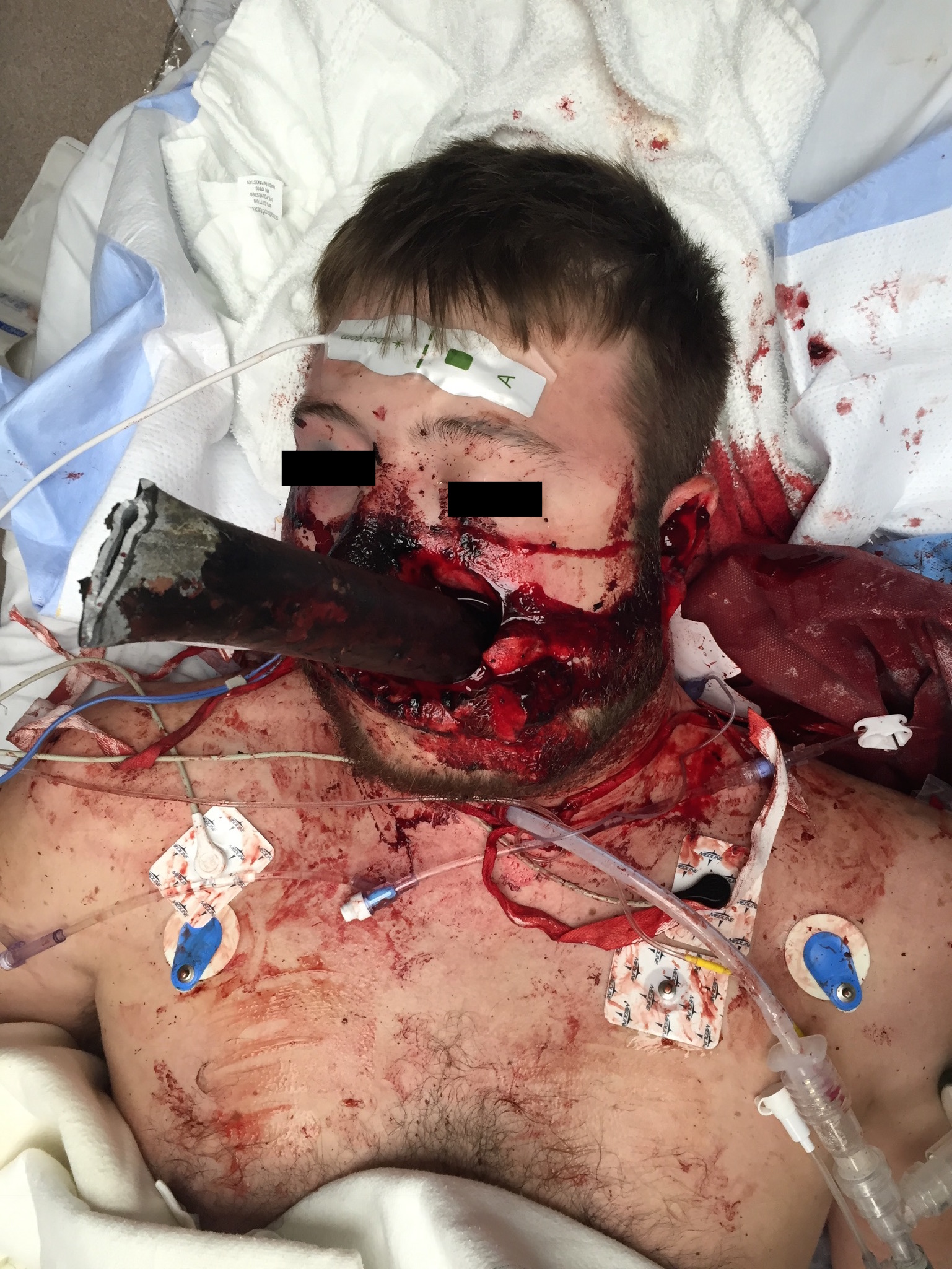
/Air Care was dispatched to a scene for a male patient in his 20s who was involved in a motor vehicle collision. Prior to arrival, first responders report that the patient was entrapped in his vehicle with a metal pole entering adjacent to his mouth and protruding out the back of his neck. There was no further information on vitals or mental status. Upon Air Care arrival, EMS had successfully extricated the patient from his vehicle by cutting the metal pole on both sides. The patient was initially combative, prompting EMS to administer 5 mg intramuscular midazolam to facilitate extrication. En route, the initial vital signs were reported to the Air Care crew as a blood pressure of 160s systolic, a heart rate of 130, and an oxygen saturation of 94% on room air. However, in the 10 minutes before Air Care’s arrival, the patient became increasingly somnolent.
Physical Exam: Initial assessment revealed a young male laying in the right lateral decubitus position on a stretcher in the ambulance. There was a moderate amount of active bleeding coming from the oropharynx and pooling on the floor of the ambulance. The EMS providers were holding a non-rebreather mask over the patient’s nose and mouth but were unable to secure it due to obstruction by the pole. His Glasgow Coma Scale (GCS) was 3, and vitals obtained by the crew were a blood pressure of 110/70, heart rate of 130, respiratory rate of 8, and an oxygen saturation of 92% on 15L. The patient had a 5 cm diameter pole entering the left side of his mouth, through his oropharynx and exiting the left posterior neck. He had ongoing intraoral bleeding but there were no other signs of head or facial trauma. Other obvious injuries included an open left forearm fracture with active bleeding. There were no external signs of trauma to his chest or abdomen. Breath sounds were diminished bilaterally, and the abdomen was soft. Peripheral pulses were present in all four extremities, and his pelvis was stable to compression.
assessing the airway
Given the active bleeding from his upper extremity, a tourniquet was immediately applied to the patient’s left arm with cessation of hemorrhage. The next priority was managing the patient’s the airway. The patient had high predicted difficulty due to multiple factors included in the “LEMON” difficult airway mnemonic (table 1).
On first look, the pole and active hemorrhage were distorting the anatomy of the face and oropharynx, making landmark identification challenging. A complete 3:3:2 evaluation and Mallampati classification of the airway were difficult to perform based on the foreign object, ongoing hemorrhage, and concern for unstable facial fractures. There was clearly a large obstruction to the airway, and neck mobility was limited due to the pole and concern for cervical spine injury. Additionally, rescue by bag-valve-mask (BVM) would be difficult as predicted by the “MOANS” assessment. The mask seal was prohibited by the patient's facial trauma and obstruction from the pole. Extraglottic device placement would also be problematic due to obstruction and likely distorted anatomy based on the “RODS” assessment. Finally, the patient did not have any true predictors of difficult cricothyrotomy based on the "SHORT" mnemonic.
the procedure
As the patient was hemodynamically stable, this was not a crash airway. Consequently, the decision was made to give one attempt at an awake look using ketamine as analgosedation with immediate transition to cricothyrotomy if unsuccessful.
Prior to the intubation attempt, the plan was verbalized to the entire team including the flight nurse and EMS providers. Specific roles were assigned to each provider. Finally, the airway equipment, suction, bougie, and cricothyrotomy kit were positioned in the appropriate places to facilitate the initial intubation attempt and potential rescue cricothyrotomy.
The awake look was attempted after administration of 150 mg of ketamine. The base of the tongue was discernible; however, visualization of the cords was difficult due to the amount of active hemorrhage, distorted anatomy, and the pole protruding through the oropharynx. Given this, the team then immediately transitioned to cricothyrotomy. After palpation of landmarks, a 4 cm vertical incision was made through the skin. Blunt dissection was performed and the cricothyroid membrane was then re-palpated to confirm location due to blood obscuring any visual landmarks.
While firmly holding the trachea, a horizontal puncture incision was made through the cricothyroid membrane resulting in bubbling of air through the pooled blood. A finger was then passed into the trachea to enlarge the incision and stabilize the trachea. With the provider’s finger still in the trachea, a bougie was passed alongside through the defect in the cricothyroid membrane. Finally, a 6.0 tube was passed over the bougie, and the cuff was inflated. This resulted in adequate end-tidal waveform and equal bilateral breath sounds. The patient was then loaded onto the helicopter and transported to the University of Cincinnati Medical Center. In route, oxygen saturations were in the mid 90s on 100% oxygen.
hospital course
Initial assessment in the resuscitation bay revealed a GCS of 3 with equal breath sounds bilaterally. Vital signs were remarkable for a systolic blood pressure in the low 100s and hypoxia to 85% on 100% oxygen. Chest x-ray showed a right mainstem intubation, so the tube was pulled back 6 cm. His oxygen saturation quickly improved to 100%. A right femoral trauma catheter was placed and two units of blood and plasma were given for borderline hypotension. CT scans were deferred due to concerns of artifact with the metal pole. The patient was taken emergently to the operating room (OR) with the trauma team, otolaryngology, and vascular surgery.
In the OR, a left neck exploration was performed which revealed intact carotid and jugular vessels. The metal pole was then removed with minimal bleeding. Additional injuries repaired in the OR included a left mandibular fracture, a right Le Fort I fracture, washout and closure of the posterior pharyngeal wound, and a complex facial laceration repair. The patient also received an open reduction and internal fixation of his left radius and ulnar forearm fractures. CT scans performed following the OR revealed numerous other injuries including multiple cervical spine transverse process fractures and an occluded left vertebral artery. A follow up MRA confirmed the vertebral artery occlusion and revealed a corresponding focal cerebral ischemic insult.
The remainder of the patient’s hospital course was uneventful. He regained consciousness and had a GCS of 15 prior to discharge. His residual neurologic deficits at discharge included paralysis of his RUE secondary to the vertebral artery occlusion and ischemia. He was discharged to an inpatient rehab facility.
discussion and post-procedural retrospective
Emergency providers are tasked with airway management on a daily basis, with the vast majority of intubations being successful on the initial attempt. Surgical cricothyrotomy is a rescue airway procedure that many hope to never have to perform, but can be life-saving when necessary. Indications for cricothyrotomy include the failure to oxygenate, failure to ventilate, or the inability to otherwise manage the airway. Success rates for surgical cricothyrotomy vary, but are generally high.[1] Details on the indications and technique of the procedure can be found in countless sources.[2] Because it is not commonly performed, providers often practice this procedure via simulations and with mental exercises. Nonetheless, these scenarios are often unrealistic when compared to the high stress situation of having to perform a cricothyrotomy on a live patient. Therefore, learning from those who have experience with this procedure can help providers prepare for the anxiety-provoking situation of the failed airway. The purpose of this discussion is to outline several practical considerations of the procedure based on the presented case.
Cricothyrotomy Truly is a Blind Procedure
The anterior neck has numerous vascular structures. Following the initial incision, blood often obstructs any further visualization of the surgical field. This makes it imperative that the provider can perform the procedure using tactile sensation only. Prior to incision, visual assessment can be performed and is helpful to locate landmarks. However, after the incision, landmarks must be palpated to identify the location of the cricothyroid membrane and allow for successful completion of the procedure.
The Trachea is Surprisingly Mobile
The trachea easily slides laterally during this procedure. Because of this, it is pivotal to have a firm grip on the trachea with the provider’s non-dominant hand to stabilize it while making the incision to expose the cricothyroid membrane. It is easy to lose the landmarks if the trachea is not properly stabilized. Additionally, while making the horizontal puncture incision in the cricothyroid membrane, stability is needed to ensure that the incision is in the proper location.
Monitor the Endotracheal Tube Depth
The distance from the vocal cords to the carina is approximately 10 cm in an adult. The distance from the vocal cords to the cricothyroid membrane is approximately 1-2 cm. Therefore, the distance from the cricothyroid membrane to the carina is approximately 8 cm.[3] When inserting the endotracheal tube, stop as soon as the balloon disappears into the trachea. This will minimize the risk of a mainstem intubation. Be aware that the tube can easily migrate and needs to be reassessed frequently. In this case, there was difficulty oxygenating in the ED due to a mainstem intubation which was likely due to migration of the tube during transport.
Communicate with Your Team
Difficult airways can be stressful for the provider, the team, and the patient. Vocalizing the airway plan for all involved is helpful to ensure that all team members know their roles and the plan going forward. Lack of knowledge that the backup plan involves a surgical airway can increase anxiety among the team members involved and lead to unnecessary errors or delays. In the case outlined above, each provider knew the initial plan and was aware of the alternative which helped to facilitate a seamless transition from the failed awake look attempt to the definitive surgical airway.
In summary, performing a surgical cricothyrotomy is one of the most stressful situations that emergency providers face. Realistic simulation for this procedure is difficult to replicate. Therefore, learning from the experience of others can help future providers save the life of the patient that cannot oxygenate, cannot ventilate, and cannot intubate.
For futher reading and videos - See Dr. Hill's Cric Page
"AirCare: To Cric or Not to Cric?" Authored by Timothy Murphy, MD
Post by Matthew Scanlon, MD
references
- Levitan, R. "A Primer On the Surgical Airway." Emergency Physicians Monthly. N.p., n.d. Web. 09 May 2017.
- Spaite, D. and Joseph, M. Prehospital cricothyrotomy: an investigation of indications, technique, complications, and patient outcome. Ann Emerg Med. 1990 Mar. 19(3):279-85.
- Powell, E., Galvagno, D., Samuel, M., Lucero, B., et al. Can’t oxygenate, can’t ventilate, can’t intubate? JEMS, 2016.
- Jenvrin J, Pean D. Cricothyroidotomy. N Engl J Med. 2008 Sept 4; 359:1073-1074.