Just the thing for the faint of heart!
/It is 3 am on a busy Friday night in your humble community ED. You have finally caught up after the evening rush of patients and are sitting down to do some charts when EMS brings in a new patient with shortness of breath. As they roll in, you see him sitting up on the stretcher, gasping for air through a non-rebreather. Placing him immediately in the resuscitation bay, you begin coordinating your staff. “Monitor, EKG, CXR, IV access!” you announce as you flip through his chart looking at his medical history. Soon your attention turns to his monitor as you hear the unmistakable beeping which is only associated with bad news.
- HR: 160, irregular
- RR:30
- BP: 90/60
- SPo2: 93% NRB
Your examination confirms your suspicion: Wet lungs, tachycardic, irregularly irregular rhythm. You’ve been here before.
You are drawing up some etomidate for a quick cardioversion when the nurse hands you his EKG. You pause for a moment, as you squint to see the QRS complexes. Those are some pretty small complexes…and do you detect a hint of alternans? Or maybe it’s just a poor baseline… You should probably take a look with the ultrasound just to be sure.
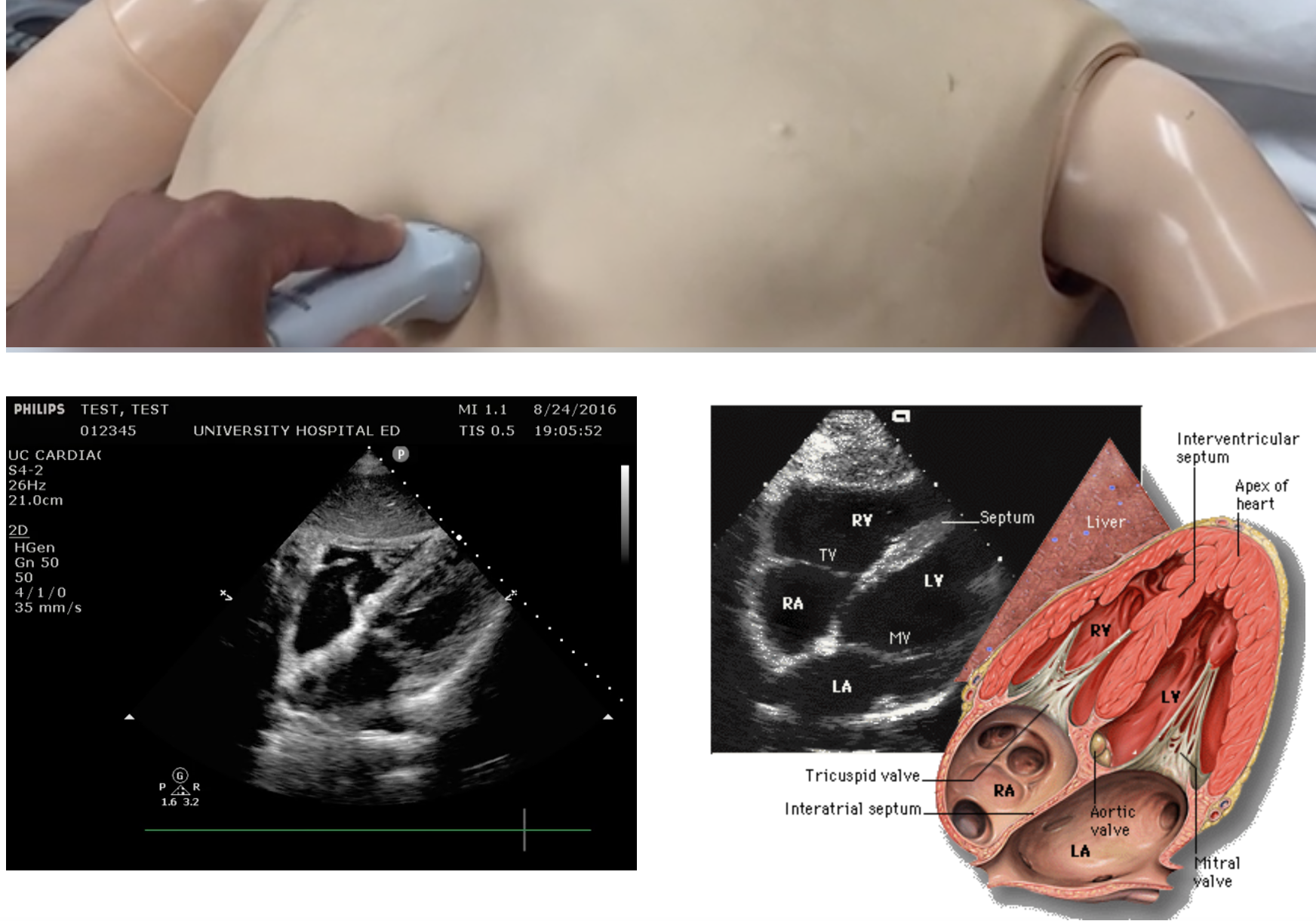
But first you head over to the dedicated Cardiac Ultrasound page for a refresher on how to perform the study!