Global Health: Case Series
/A common RASH IN RURAL TANZANIA
Imagine you are a provider working in a rural clinic in Tanzania near Lake Victoria...
Your next patient is a family of five, a mother in her 20s and children ranging in age from seven years to nine months old, all complaining of body rashes. The mother reports that the rash initially started with the school age children and has since spread to other members of the family. The children describe the rash as itchy, but not painful. Initially the rash was worst on the hands but has since spread to the rest of the body. All family members deny any other symptoms including fevers, headache, nausea, vomiting, or joint pain. Although family has had limited access to healthcare the mother does not know of any medical problems among herself or the children.
Vital signs of the family are within normal limits
Shared Physical Exam
General: Well appearing, in no acute distress
HEENT: PERRL, EOMI. Oropharynx clear. Mucous membranes without lesions
Cardiac: Regular rate and rhythem, no murmurs
Pulmonary: Lungs clear without any wheezes, rhonchi or rales
Abdomen: Soft, nontender, nondistended
Extremities: No tenderness to palpation, full range of motion of upper and lower extremities bilaterally. No edema.
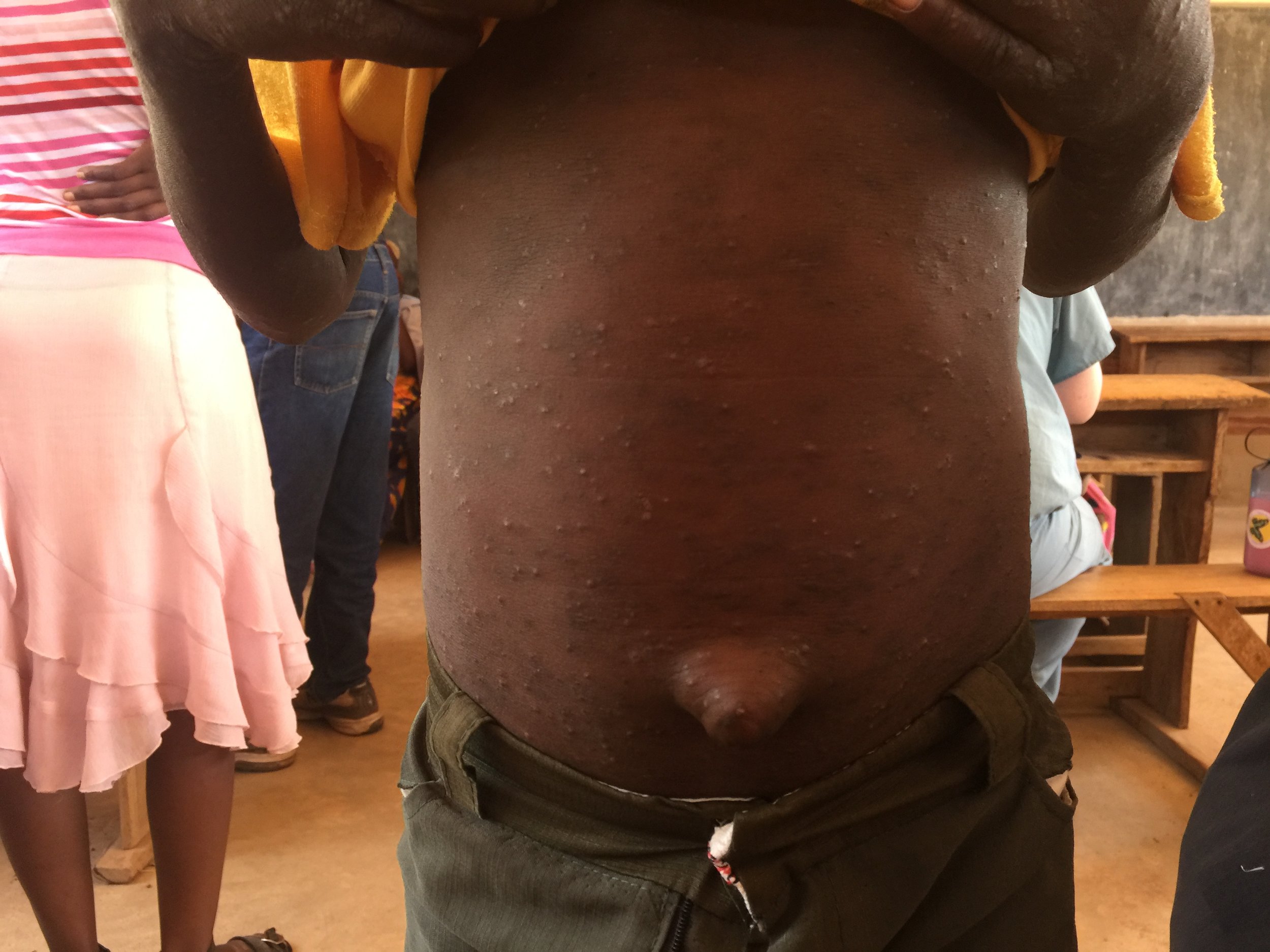
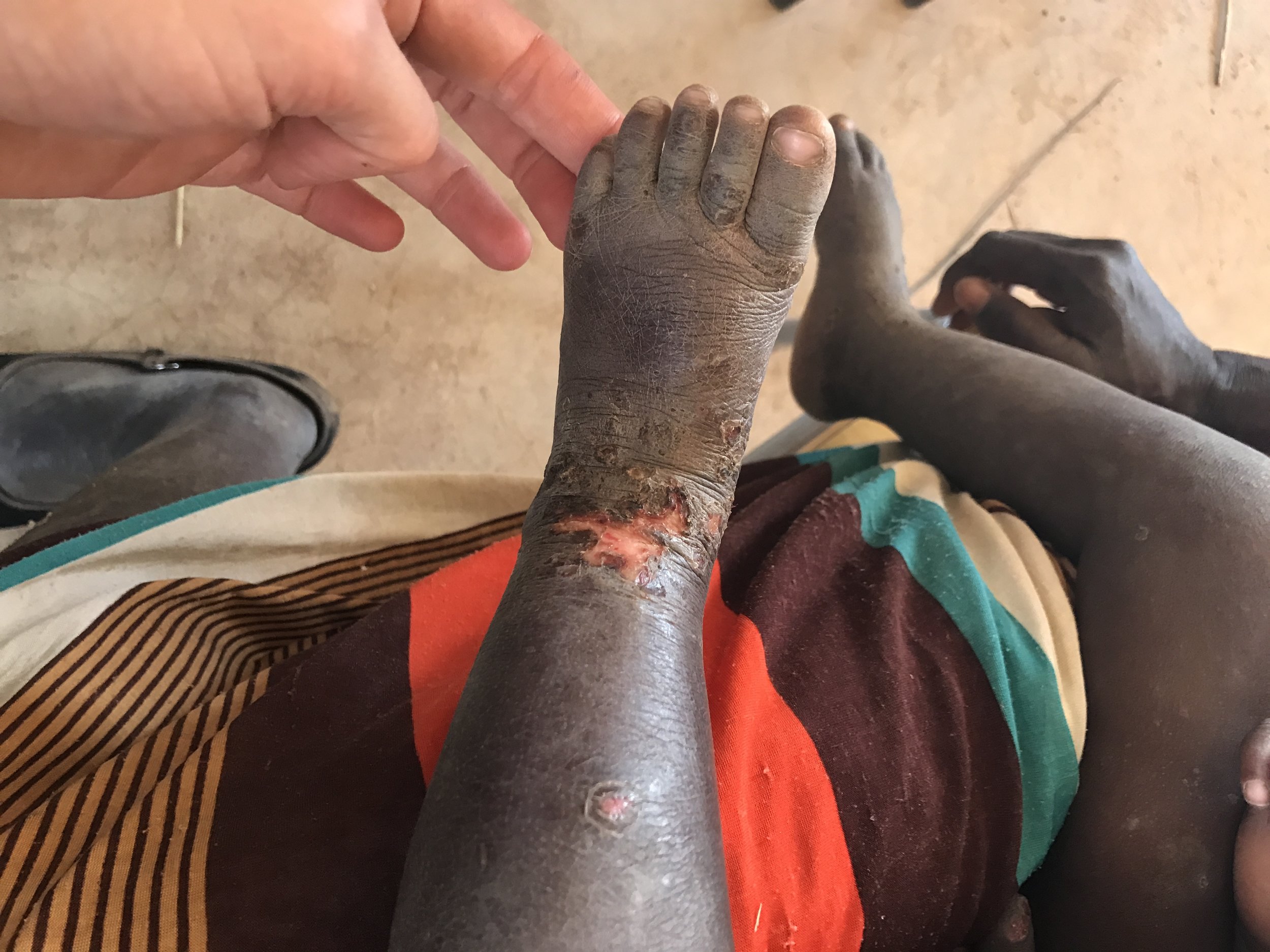
Skin: Multiple scattered erythematous papules with multiple surrounding excoriations and hemorrhagic crusts, mostly localized to extremities but also present on trunk
+ What is the Most Likely Diagnosis?
SCABIES
You may have recognized the characteristic findings of scabies from the history and physical exam. This case was not a diagnostic dilemma. What it does highlight is the dilemma of how to treat patients when you do not have access to medications that are considered first or second line treatment.
Scabies is an infection caused by the skin mite Sarcoptes scabiei. The scabies mites burrow into the epidermis by secreting proteolytic enzymes resulting in keratin damage, which causes an intensely pruritic rash. Scabies is spread by prolonged skin-to-skin contact, often greater than 10 minutes, or by contact with infected clothing, bedding, or furniture. The first sign is often an intense itch that usually begins in the web space between fingers or in the genital area. Later the rash can spread diffusely but often excludes the head in adults. However, in infants and young children head involvement is very common. The rash usually consists of scattered small erythematous papules that often become hemorrhagic crusts due to frequent excoriation. Burrows may be visible as 2 to 15 mm thin grey or red lines in the web spaces between fingers. Secondary excoriation or infection can obscure a provider's ability to view burrows but, if visualized they are diagnostic.
In the United States, the most common treatment for scabies is permethrin cream. Permethrin cream is applied to the whole body and treatment should be repeated in 1 week. Treatment should be given to all household contacts even if they do not have signs or symptoms of scabies. A review of randomized controlled trials concluded that permethrin was the most effective agent for treatment of scabies. For severe cases or in patients who have failed permethrin, oral ivermectin has also been shown to be very effective. Oral ivermectin should be taken in two doses one week apart. It is important to know that oral ivermectin as treatment for scabies is not FDA approved.
Although the treatment of scabies may seen straight forward, in resource-limited areas treating scabies can be very challenging. Difficulties often arise when providers do not have access to first or second line treatment options. Additionally, a patient’s scabies can be very severe due to superimposed bacterial infections from frequent excoriation.
Because scabies is spread by close contact, crowded living conditions increase the risk of scabies infestation. The World Health Organization (WHO) reported a world-wide prevalence of scabies ranging from 0.2-24% with the highest prevalence occuring in India, South Pacific, northern Australia and Latin America.
In Shirati, Tanzania, where this case occurred, there was no available permethrin cream or oral ivermectin. After discussing treatment options with local providers in the area, alternative treatments were identified. Sulfur based soaps and ointments were widely available and are one of the oldest known treatments of scabies. Sulfur based treatment for scabies is also safe to use in the pediatric and pregnant populations. Sulfur based treatments are most efficacious when used for 3-4 consecutive nights. Sulfur treatments are not commonly used when alternative therapies are available due to their odor and difficultly in applying topically which can cause clothing stains. Benzyl benzoate, an ester of benzoic acid and benzyl alcohol, is another treatment option that acts as a neurotoxin to the mites. The main limitation with this treatment is skin irritation as it can cause significant burning with application. Because of this the dosage may need to be reduced for children and young adults. However, in some populations, benzyl benzoate as been found to be effective against permethrin resistant scabies.
Untreated scabies in immunocompromised patients can lead to the development of severe form of scabies called crusted scabies. This is thought to be due to uncontrolled proliferation of mites in the skin. Crusted scabies can be resistant to many topical treatments and often requires multiple rounds of oral ivermectin treatment. If a patient presents with crusted scabies, providers should consider additional work up for HIV and other immunocompomising diseases.
For the above reasons scabies remains difficult to treat in resource-limited settings. The strategy of treating only clinical cases and close contacts often provides relief for individuals, but has not been shown to reduce prevalence among populations with a high burden of disease. Mass drug administration with oral ivermectin has been utilized in certain communities with better results. Mass treatment was given in the Solomon Islands in 2000 and reduced prevalence from 25% to 1%. Until mass treatment becomes widely employed, factors contributing to community wide decrease in scabies continues to hinge on education and treatment for infected individuals and all close contacts.
Authored by Kathryn Banning, MD
Posted by Grace Lagasse, MD
References
1. Goldstein, B. (2017). Scabies: Epidemiology, clinical features, and diagnosis. UpToDate.
2. CDC guidelines: Scabies. (2017)
3. Hay, R., et al. (2012) Scabies in the developing world – its prevalence complications, and management. European Society of Clinical Microbiology and Infectious Disease. 18(4) 314-323. doi: 10.1111/j.1469-0691.2012.03798.x