Flights - A Stab in the Dark - Curated Comments and Expert Commentary
/Thanks to everybody who contributed to an excellent discussion of the care of the patient on our second “flight.” If you didn’t get a chance to check out the case and the discussion, check it out here. Below is the curated comments from the community and a podcast from Dr. Hinckley and Flight Nurse Practitioner Jason Peng.
Q1 - Walk through your initial assessment of this patient. What are the critical aspects of the assessment of this patient?
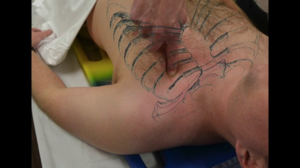
In response to this question, most everybody wanted to first act on the bleeding wound in the patient’s right antecubital fossa. As explained by Dr. Renne, “I would want to be systematic but efficient, probably using a C-ABCD approach to these kind of critical patients, with the first C being any sort of life-threatening but "C"ontrollable hemorrhage.” Dr. Renne also had a fine point with regards to checking for other potential, as of yet unseen, injuries. This is a patient with multiple stab wounds, it is crucial to conduct a quick, but thorough search for stab wounds to the back, axilla, groin, and/or other locations where significant blood loss could be caused by a stab wound.
With regards to the patient’s hemodynamics, most everyone felt the patient was in hemorrhagic shock and also had the potential to have superimposed tension pneumothorax pathophysiology. As stated by Dr. Gorder, “My bet is that her tachycardia and hypotension is from tension physiology more so than acute blood loss…” As will be seen in the answers to question 2, focusing in on the blood loss, decreased breath sounds, hypotension and tachycardia, made addressing B (breathing) and C (circulation) a priority for everyone.
Q2 - Do any procedures need to be performed on this patient? If so, who performs the procedures? In what order should they be done? Where do you do these procedures (squad/in flight/receiving hospital)?
Judging by the responses from the community, there is much to be done for this patient.
The first procedure on most everybody’s list was placing a tourniquet on the right upper extremity. With bleeding uncontrolled by direct pressure and the need to have as many free hands as possible in-fight, placing a tourniquet is a great idea. Dr. Ludmer brought up the possibility of using Combat gauze as a temporizing measure in this patient before placing a tourniquet. As pointed out by Dr. Hinckley, even with a tourniquet in place to stop arterial bleeding, it may be necessary to use a hemostatic gauze to help stop venous bleeding.
Additional access was also a priority for the crew. Contributor Scott Long noted, that could be a peripheral IV or could be an IO: “Next have medic, nurse someone familiar start second line/ Left humeral head IO and once completed begin FFP/ PRBC infusion( possible hypemic hypoxia)”
A Needle or Finger to Free Trapped Air
Next up on the to-do list was performing a needle thoracostomy with consideration for finger thoracostomy. As described by Dr Gorder, “I would start with a needle decompression, as I feel it’s a quicker procedure (for me, at least, in this point in my training) than an on-scene finger thoracostomy and I would be wanting to get this patient moving as fast as possible.” For more information about needle and finger thoracostomies check out these posts from last years curriculum:
Needle to the Heart or Not?
Given the penetrating injury to the chest wall, several people were rightly concerned about the possibility of pericardial tamponade. While not necessarily inclined to perform this procedure on the first pass of treatment of the patient, most providers wanted to monitor the patient’s response to volume resuscitation, the tourniquet, and the needle/finger thoracostomy before heading towards pericardiocentesis. Dr. Ludmer makes a nice point about the location of the wound, I think my decision to perform a pericardiocentesis would depend greatly on the location of the wounds, “If the wounds were largely right sided, I would be less inclined to perform the procedure. I think once the tourniquet was applied, access was established, blood was hung, and needle decompression was performed, I would probably begin transport and monitor for improvement in blood pressure.”
On Airway Management
There was understanding and acceptance that this patient may eventually require RSI, though everybody agreed the patient required a degree of resuscitation before the procedure would be attempted. As described by Dr. Gorder, “It would probably take a lot for me to intubate this patient. I discussed a similar hypothetical case with Dr. Stull a few nights ago in B-Pod, and he raised some great points about intubating penetrating trauma patients. In this case, I feel it is safe to assume that the patient’s change in mental status is due to her hemodynamics, and not a head injury. If she remains hypotensive and/or altered after we fix her likely PTX, it’s product she needs. RSI and intubation could drop her already tenuous preload and cause her to arrest in front of us.”
The logistics of when and where RSI would occur is still somewhat in question. Shad Ruby noted, “A few have mentioned deferring airway management. So a couple things to consider. Capturing the airway can be much more difficult in the aircraft. That is not to say it can't happen, especially with VL, but it has to be considered. I believe I would most likely do it before transport.”
Q3 - What medications should be used in the care of this patient? Should this patient receive blood products? If so, what type and in what order?
The community resoundingly supported the administration of blood products and TXA for the patient. As stated by Drs. Plash and LaGasse, “We would give this patient TXA, 1gm over 10 minutes. We would also give her blood products specifically 1:1 pRBCs and FFP for her hemorrhagic shock.”
There were several options brought up with regards to the administration of analgesic medication in this patient. Dr. Teuber was inclined to choose to administer small aliquots of fentanyl, paying close attention to the hemodynamic effects of the medication. Several contributors brought up the possibility of using ketamine for analgesia in this patient. As noted by Dr. Hinckley, Air Care and Mobile Care protocols do not currently include the administration of ketamine for pain or procedural sedation (ONLY induction). As such, if it is felt that ketamine is the most ideal agent for analgesia or procedural sedation, a flight doc or nurse will need to call medical control first.
Q4 - Given the environmental conditions, what additional steps should be taken in the care of the patient?
Rick Jamie brought up excellent points in considering the environmental conditions. After briefly exposing to look for other injuries and performing any procedures that require exposure, getting the patient bundled in blankets and using the fluid warmer for blood products will be crucial in preventing hypothermia. He also brought up several excellent points with regards to the logistics of packaging a patient, “while placing cabling and IV lines in a configuration that allows for easy access, decreases possibility of pinched lines, and secure the pt while keeping her warm.... Pinched off IV lines don't deliver warm products... May sound like a simple or insignificant item, but a couple of extra seconds to manage cabling and lines can make a difference!”
Expert Commentary
For this recap, Dr. Hinckley is joined by Flight NP Jason Peng who has >15 years of EMS experience and has been with ACMC since 2011. They sat down with Dr. Hill to talk over their approach to this latest case.