Intern Diagnostics: Corneal Pathology
/Ophthalmologic complaints encompass 1.5% of total emergency department visits, with diseases of the cornea accounting for some of the most common. In this post, we will review four of the most common corneal pathologies as well as their acute management from the emergency department perspective.
The Cornea
The cornea is the most anterior structure of the eye. It performs the initial refraction of light onto the lens, and it acts a barrier between the internal structures of the eye and the outside world. The cornea is innervated by the ophthalmic branch of the trigeminal ganglion, and has 300-600 times the nociception of skin.
The cornea is divided into five distinct layers:
Epithelium
Bowman’s membrane
Stroma
Descemet’s membrane
Endothelium
Keratitis
This refers to inflammation of the cornea from any source. Keratitis is associated with corneal edema, the migration of inflammatory cells, and congestion. There are numerous causes of keratitis, which can be divided into infectious and non-infectious etiologies.
Infectious: Most commonly bacterial (Staphylococcus, Streptococcus, Pseudomonas), but can also be viral (HSV, VZV), fungal (Aspergillus, candida), or protozoal (acanthamoeba)
Non-Infectious: UV keratitis, peripheral ulcerative keratitis, xeropthalmia, neurotrophic corneal ulcers
Abrasions and ulcers are rwo pathologies that involve damage to the corneal epithelium are corneal abrasions and corneal ulcers, which together make up 13% of ophthalmologic emergencies.
Corneal Abrasion
Corneal abrasions are defects that are more superficial, only involving the epithelial layer of the cornea. Abrasions are typically the result of superficial trauma, such as from fingernails, debris, or contact lenses, but can also occur spontaneous particularly in patients with diseases causing dry eye. Corneal abrasions should be treated with topical antibiotics, typically erythromycin or ciprofloxacin for contact lens wearers to cover for pseudomonas.
| Definition | History | Treatment | Ophtho Consult? | |
|---|---|---|---|---|
| Abrasion | Epithelium | Acute, trauma | Topical erythromycin | No |
| Ulcer | Stroma + infiltrate | Insidious onset | Stronger topical abx/antivirals | Yes |
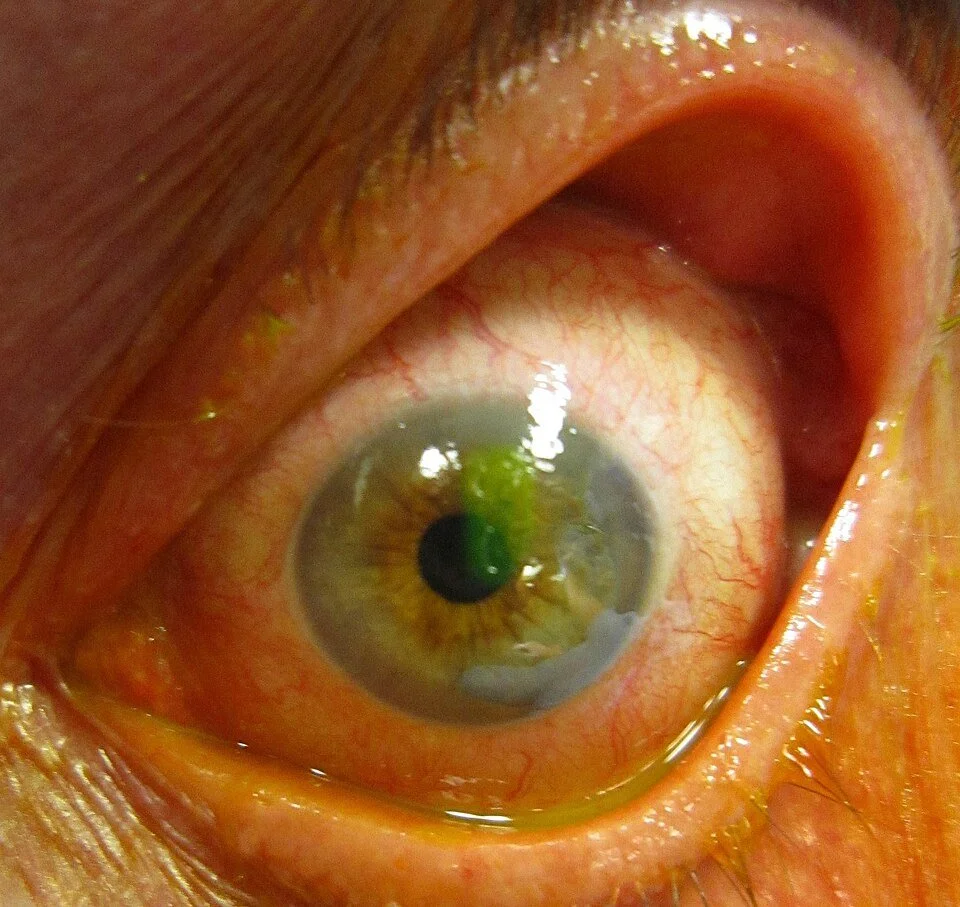
Corneal Ulcer
Corneal ulcers also involve the epithelium, however they also extend through Bowman’s membrane into the stroma. Corneal ulcers typically begin as keratitis, and a break in the epithelium allows for microbial entry. The most common pathogens are consequently the same pathogens that cause keratitis, detailed above. As corneal ulcers are typically from an infectious source, corneal scraping for culture and sensitivities is an important part of the workup performed by ophthalmology. Corneal ulcers are typically treated with topical antibiotics or antivirals depending on anticipated etiology. In the emergency department, it is important to look at previous culture data for patients with recurrent ulcers. Certain etiologies such as gonococcus may require admission for IV antibiotics. Topical steroids have mixed utility, and decisions regarding the timing of their addition are typically left to ophthalmology and are dependent on sterility.
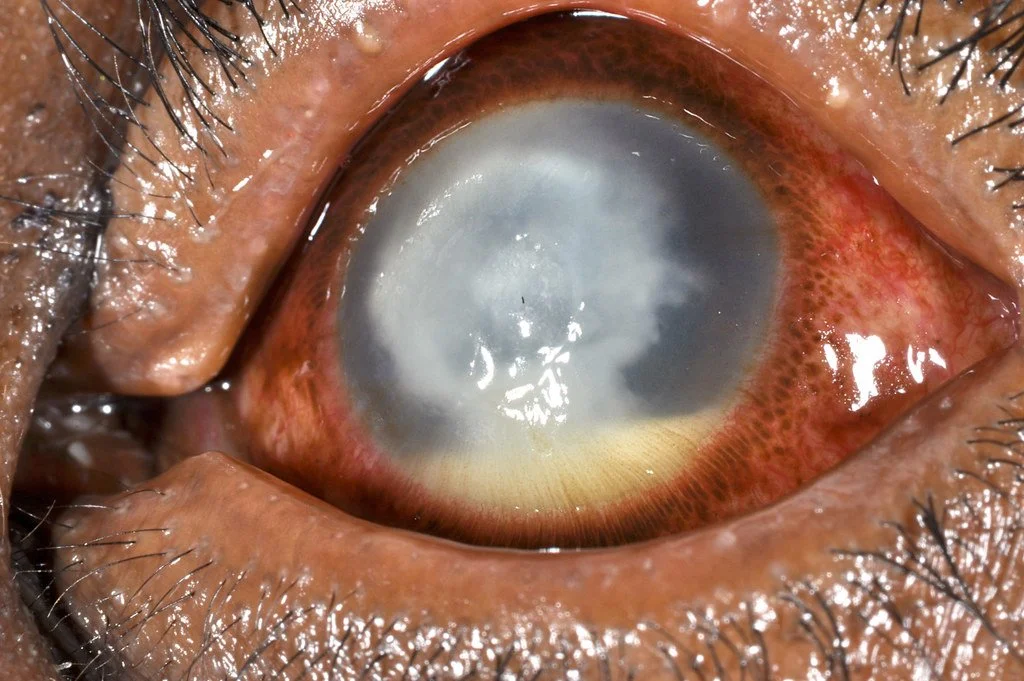
Endophthalmitis
Endophthalmitis denotes a purulent inflammation of the intraocular fluids, both aqueous and vitreous. Endophthalmitis most commonly occurs post-operatively, especially after cataract surgery, but also can occur after trauma or from endogenous spread. The vast majority of cases are due to gram positive bacteria, with the most frequent isolate being staph epidermidis. The hallmark physical exam finding of endophthalmitis is a hypopyon, which is a collection of white blood cells in the anterior chamber of the eye. Endophthalmitis can also be associated with more systemic symptoms, so blood cultures can be valuable. Treatment involves intravitreal injections of antibiotics and possible vitrectomy.
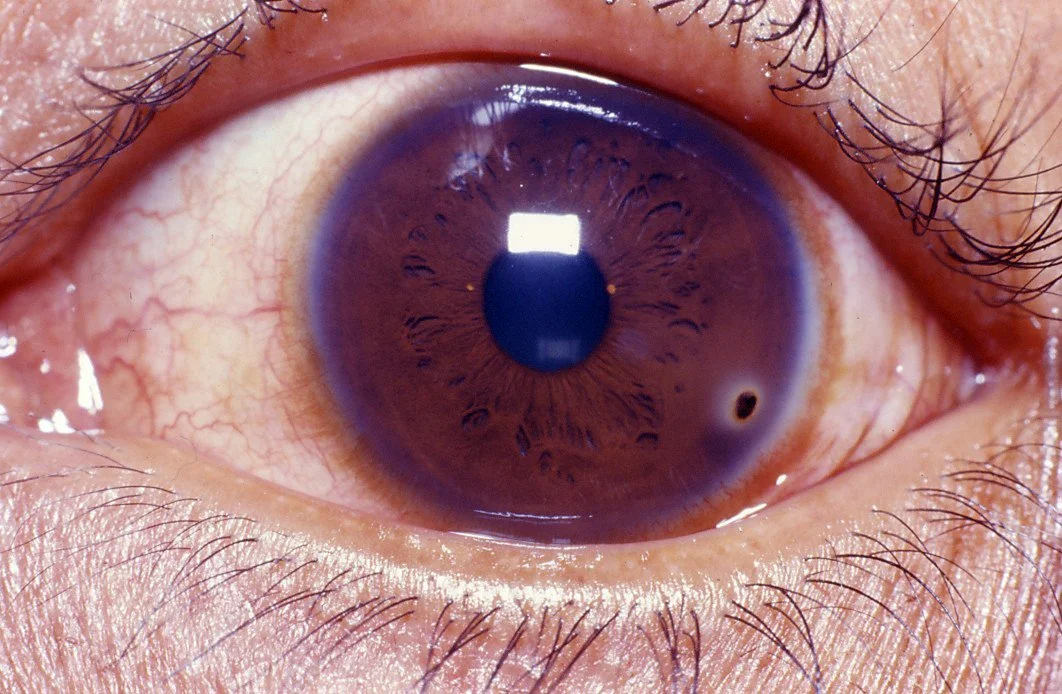
Corneal Foreign Body
Foreign bodies can lodge in any layer of the cornea. Specific considerations should be taken to address the nature of the foreign body itself. For example, organic material is associated with a higher risk of infection, metallic foreign bodies and leave a rust ring on the cornea, and the presence or absence of contact lenses can necessitate broader antibiotic coverage. Fluorescein exams are useful for detecting superficial foreign bodies and associated abrasions, whereas orbital CT scans may be useful for more deeply embedded objects or suspected penetrating objects. A notable physical exam finding is hyphema, or a collection of red blood cells in the anterior chamber, which indicates globe perforation. Globe perforation can also be detected on fluorescein exam with a positive Seidel sign. If there is concern for globe perforation, an ophthalmologist should be consulted immediately.
All foreign bodies should receive a thorough slit lamp exam, including examination of the entire eye, lash line, and upper eyelid. Multiple removal techniques can be utilized including irrigation, a damp cotton swam, a 25-30 gauge bevel of a needle, or a corneal burr. After extraction, patients should receive prophylactic topical antibiotics, a Tdap vaccination, and lubricating eyedrops.
References
Emami S, Kitayama K, Coleman AL. Adjunctive steroid therapy versus antibiotics alone for acute endophthalmitis after intraocular procedure. Cochrane Database Syst Rev. 2022;6(6):CD012131. doi:10.1002/14651858.CD012131.pub3
Al-Mujaini A, Al-Kharusi N, Thakral A, Wali UK. Bacterial keratitis: perspective on epidemiology, clinico-pathogenesis, diagnosis and treatment. Sultan Qaboos Univ Med J. 2009;9(2):184-195.
Gurnani B, Kaur K. Bacterial Keratitis. In: StatPearls. StatPearls Publishing; 2025.
Ahmed F, House RJ, Feldman BH. Corneal Abrasions and Corneal Foreign Bodies. Prim Care. 2015;42(3):363-375. doi:10.1016/j.pop.2015.05.004
Beyer H, Cherkas D. Corneal foreign body removal using a bent needle tip. Am J Emerg Med. 2012;30(3):489-490. doi:10.1016/j.ajem.2010.12.038
Arbabi EM, Kelly RJ, Carrim ZI. Corneal ulcers in general practice. Br J Gen Pract. 2018;68(666):49-50. doi:10.3399/bjgp17X694385
Shah A, Blackhall K, Ker K, Patel D. Educational interventions for the prevention of eye injuries. Cochrane Database Syst Rev. 2009;2009(4):CD006527. doi:10.1002/14651858.CD006527.pub3
Sadiq MA, Hassan M, Agarwal A, et al. Endogenous endophthalmitis: diagnosis, management, and prognosis. J Ophthalmic Inflamm Infect. 2015;5(1):32. doi:10.1186/s12348-015-0063-y
Durand Marlene L., Barshak Miriam B., Sobrin Lucia. Eye Infections. New England Journal of Medicine. 2023;389(25):2363-2375. doi:10.1056/NEJMra2216081
Vaziri K, Schwartz SG, Flynn HWJ, Kishor KS, Moshfeghi AA. Eye-related Emergency Department Visits in the United States, 2010. Ophthalmology. 2016;123(4):917-919. doi:10.1016/j.ophtha.2015.10.032
Ozkurt ZG, Yuksel H, Saka G, Guclu H, Evsen S, Balsak S. Metallic corneal foreign bodies: an occupational health hazard. Arq Bras Oftalmol. 2014;77(2):81-83. doi:10.5935/0004-2749.20140020
Results of the Endophthalmitis Vitrectomy Study. A randomized trial of immediate vitrectomy and of intravenous antibiotics for the treatment of postoperative bacterial endophthalmitis. Endophthalmitis Vitrectomy Study Group. Arch Ophthalmol. 1995;113(12):1479-1496.
Quintero M, Mahjoub H, Ssekasanvu J, et al. Sociodemographic Factors Associated With Emergent Eye-Related Emergency Department Visits: A Multicenter Analysis. Am J Ophthalmol. 2025;269:84-93. doi:10.1016/j.ajo.2024.06.031
Rabin E, Patrick L. Specialist availability in emergencies: contributions of response times and the use of ad hoc coverage in New York State. Am J Emerg Med. 2016;34(4):687-693. doi:10.1016/j.ajem.2015.12.059
Wedekind L, Sainani K, Pershing S. Supply and Perceived Demand for Teleophthalmology in Triage and Consultations in California Emergency Departments. JAMA Ophthalmology. 2016;134(5):537-543. doi:10.1001/jamaophthalmol.2016.0316
Belmonte C, Nichols JJ, Cox SM, et al. TFOS DEWS II pain and sensation report. Ocul Surf. 2017;15(3):404-437. doi:10.1016/j.jtos.2017.05.002
Srinivasan M, Mascarenhas J, Rajaraman R, et al. The steroids for corneal ulcers trial (SCUT): secondary 12-month clinical outcomes of a randomized controlled trial. Am J Ophthalmol. 2014;157(2):327-333.e3. doi:10.1016/j.ajo.2013.09.025
Prakash G, Avadhani K, Srivastava D. The three faces of herpes simplex epithelial keratitis: a steroid-induced situation. BMJ Case Reports. 2015;2015:bcr2014209197. doi:10.1136/bcr-2014-209197
Green SM, Tomaszewski C, Valente JH, Lo B, Milne K. Use of Topical Anesthetics in the Management of Patients With Simple Corneal Abrasions: Consensus Guidelines From the American College of Emergency Physicians. Ann Emerg Med. 2024;83(5):477-489. doi:10.1016/j.annemergmed.2024.01.004
Negretti GS, Chan W, Pavesio C, Muqit MMK. Vitrectomy for endophthalmitis: 5-year study of outcomes and complications. BMJ Open Ophthalmol. 2020;5(1):e000423. doi:10.1136/bmjophth-2019-000423
Paterson R, Drake B, Tabin G, Cushing T. Wilderness Medical Society Clinical Practice Guidelines for Treatment of Eye Injuries and Illnesses in the Wilderness: 2024 Update. Wilderness & Environmental Medicine. 2024;35(1_suppl):67S-77S. doi:10.1177/10806032231223008
Cite As: Carroll K., LaFollette R. Intern Diagnostics: Corneal Pathologies. TamingtheSRU. www.tamingthesru.com/blog/diagnostics/corneal-pathology
Post by Katie Carroll, MD
Dr. Carroll is a PGY-1 in Emergency Medicine at the University of CIncinnati
Peer Editing and Post by Ryan LaFollette, MD
Dr. LaFollette is an Assistant Program Director and co-editor of TamingtheSRU.com